New Patients
Get Started With Us
Patient Portal
Existing Patients
Current Specials
Deals and specials
Get Started With Us
Existing Patients
Deals and specials
Mohs micrographic surgery, which is performed in the office using local anesthesia, is a state-of-the-art treatment for skin cancer in which the physician serves as a surgeon, pathologist, and reconstructive surgeon. It yields the highest cure rate of all skin cancer treatments, with cure rates approaching 99% for tumors that have not previously been treated. The procedure relies on the precision and accuracy of examining tissue under a microscope to trace and ensure removal of the skin cancer, which may have roots that extend beyond what is visible to the naked eye. In addition, the removal of healthy skin is minimized, resulting in the smallest possible surgical defect and thereby decreasing the potential for scarring.
The most common types of skin cancer are BASAL CELL CARCINOMA and SQUAMOUS CELL CARCINOMA. Both of these types of skin cancer enlarge over time but usually do not metastasize (move to different areas of the body). Squamous cell cancers of the lip, ears and nose have a higher rate of metastasis and because of this, need to be followed closely after surgery. If the cancers are not completely removed they can invade and destroy adjacent structures such as the eye or nose. Compared to other forms of cancer, these types of skin cancer are generally recognized in their early stages and more easily cured. If left untreated skin cancers will form a non-healing ulcer, which may gradually enlarge.
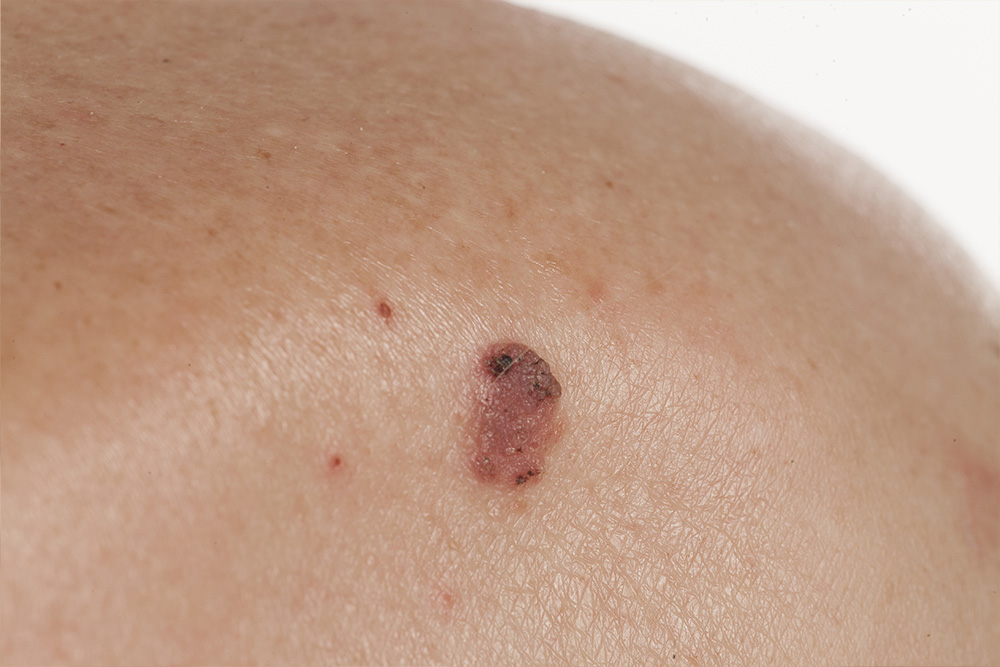
MALIGNANT MELANOMA on the other hand may be life threatening if not treated early. It usually appears as a brownish-black spot or bump on the skin, which enlarges and sometimes bleeds. Melanomas can originate in moles that have been present for many years. If you find a suspicious looking mole, please have your referring physician, refer you to Dr. Darlene S. Johnson, Dr. Misha Miller or Dr. Jamison Strahan to examine it as soon as possible.


The cause of skin cancer, like other forms of cancer, is not completely known. Excessive exposure to sunlight is the single most important factor associated with the development of skin cancers, which appear most commonly on the face and arms (the most sun-exposed parts of the body). Fair skinned people tend to develop skin cancer more frequently than dark skinned people. Skin cancers are more common in the southern and Rocky Mountain states. Skin cancer also tends to be seen more often within certain ethnic groups, such as English, Scottish, Irish and Scandinavians. Thus, the tendency to develop skin cancer is inherited along with your complexion. However skin cancers are certainly not limited to these ethnic groups and are routinely treated in all ethnic groups.
Skin cancer begins in the uppermost layer of the skin and grows downward forming roots and spreading horizontally along the surface of the skin. One can compare the skin cancer growth to a plant. There is visible result on the surface of the skin, but underneath is a complex root system that is impossible to know exactly where it extends. Therefore, what is apparent to the naked eye may only be the “tip of the iceberg”.
There are several methods of treating skin cancer, all very successful in the majority of the patients.
These methods include:
• Excision and suturing (surgical removal and stitches)
• Curettage and electrodesiccation (scraping and burning with an electric needle)
• Cryosurgery (freezing)
• Mohs Surgery (microscopically controlled excision)
The method chosen depends on several factors, such as location, size, severity, and previous treatment of skin cancer.
The types of skin cancers that are most often treated by Mohs Surgery include the following:
• Cancers on or around the nose, ears or eyes, which have or have not been treated before.
• Cancers which have been treated before but have recurred.
• Cancers which have a scar-like appearance and feel.
• Cancers with a hard to judge border.
• Some types of skin cancers in younger patients.
There are many advantages to using Mohs Surgery. The first and foremost is that it assures complete removal of the skin cancer, while preserving as much normal skin as possible. The surgery is performed in an office setting, thus avoiding operating room and hospital fees. It is also much more relaxing.
The surgery is safe, reliable and has a significantly higher cure rate than any other available technique, even when dealing with the most difficult tumors. Mohs Surgery has a cure rate approaching 99% for tumors that have not been treated in the past. For skin cancers that have been previously treated but recurred, the cure rate for Mohs is around 95%. Therefore, an excellent chance of cure is achieved, however, no one can guarantee a 100% cure.
Mohs surgery is performed in an office setting under local anesthesia. The skin that appears to be involved in the tumor is removed, color-coded and mapped out for later identification and orientation under a microscope. After laboratory preparation the entire periphery and undersurface of the specimen is examined microscopically to detect any residual cancer. If cancerous cells remain, more skin is removed, but only from the area where the cancer was seen. The skin is then prepared in the same way and this process is repeated as many times as necessary until the area is cancer free.
Dr. Darlene S. Johnson, Dr. Misha Miller, and Dr. Jamison Strahan are Board Certified Dermatologists and have done fellowships in Mohs Surgery. This is a one year program. Not all dermatologists are trained to perform Mohs Surgery. This is a highly skilled procedure and a trained histotechnician must also be on site to do the lab work.
Each stage of the surgical procedure takes about 15-20 minutes to remove the area of cancer. Following the removal, it takes about an hour and a half for the slides to be prepared and examined. Several surgical stages and microscopic examinations may be required. For this reason, please bring reading material or something to occupy your time while you wait on the day of your surgery. It is also a good idea to bring someone with you or at least have someone “on call” to drive you home if necessary. Due to limited space in our office, please limit yourself to bringing only one person.
It is very important that you set aside the entire day. This is because some surgeries require several stages and predicting exactly when we will be done is not possible. We also request that after the surgery you go home and rest.
Please remember that the above times are only guidelines. Sometimes we do run later than anticipated, for example if a cancer is larger and requires more sections or if you have multiple skin cancers being treated by Mohs. In any case we will keep you informed of the progress.
Try to get a good night’s sleep and eat a light breakfast. If you are taking any medication take it as usual unless we direct you otherwise.
We do ask that you let us know of any medications that you are currently taking or are allergic to, especially any local anesthetics such as xylocaine. Certain medications, even over-the-counter medications, can cause complications with the surgery. We ask that aspirin containing products be discontinued 7 days prior to surgery. These products tend to prolong bleeding during surgery. If you are taking aspirin under the advice of your physician to prevent strokes or blood clots, please get their OK prior to discontinuing and inform us of their decision. If your physician feels strongly that you should stay on aspirin we can then anticipate potential problems.
Please let us know if you are taking any prescription blood thinners such as Coumadin. It may cause excessive bleeding, but in most cases you will not have to discontinue the drug prior to surgery.
Other over-the-counter medications can prolong bleeding. Ibuprofen should be discontinued for 7 days prior to surgery. See the attached Medication Precaution guide. Even some herbal supplements, such as Ginkgo Biloba and Vitamin E should be discontinued for 7 days prior to surgery due to their blood thinning effect.
If your physician requires that you be placed on an antibiotic prior to surgery please let us know. This pertains to individuals who have artificial joints or heart valves and also individuals with a previous history of rheumatic fever.
There are some supplies that you may wish to pick up prior to your surgery so that you don’t have to go out the evening after your surgery. The supplies you will need are:
You should not drive if you are taking a prescription strength pain medicine. If you need to drive, operate machinery or simply wish to avoid taking pain medications you may take Extra-Strength Tylenol.
Please select comfortable clothing that won’t require you to pull over your head. Women should not wear make-up if they are having surgery on any area of the face.
Please turn off your cell phone while in the surgical room.
Please remember that your questions and concerns are very important to us. If at any time you have a question concerning the procedure please let us know and we will address it to the best of our abilities.
We will use a local anesthetic, usually Lidocaine, to numb the cancer and the surrounding skin. Be sure to inform us if you experience anything more than a slight discomfort. If, while you are waiting between stages and you start to have any pain let us know. We can either re-inject the area or give you a pain medication.
All appointments for Mohs Surgery are scheduled early in the day. This allows us to continue throughout the day. If you are a new patient to Advanced Dermatology, we ask that you arrive 10 minutes early to complete the required paperwork. All patients will be required to complete a consent form for Mohs Surgery stating that you understand the complications of the surgery. Dr. Johnson/ Dr. Miller/ Dr. Strahan will examine the cancer and trace its visible border with a skin marker.
The site is then injected to numb the entire area. After allowing thorough penetration of the Lidocaine,
Dr. Johnson/ Dr. Miller/ Dr. Strahan cuts out an area of the skin cancer. After removal, local bleeding is stopped by means of cautery. If you have any medical reasons that a cauterizing machine should not be used, please let us know. Before you leave the surgery room, the nurse will dress your wound with a pressure dressing. The area of the skin that was removed is labeled and given to the technician. If examination of the slides reveals that your tissue still contains cancer cells then the procedure is repeated as soon as possible.
It is a good idea to bring a lunch or some snacks for the day. We have a small refrigerator that you may use. Beverages and an assortment of snacks are available for our Mohs patients. Please feel free to serve yourself.
Most patients state that there is some pain the night of the surgery. For this reason, Dr. Johnson/ Dr. Miller/ Dr. Strahan will write a prescription for pain medication for you to take once you get home and throughout the night. If you are allergic to any medications please let the nurse know.
Rarely does bleeding occur following surgery. We will give you extensive postoperative instructions following the surgery and ask that you follow them. By following the instructions on the sheet you will greatly minimize your chance of having bleeding following the surgery. We will also give you instructions on what to do if bleeding does occur.
For the week following your surgery there will be limitations placed upon your activity. We ask that you do not exercise or do any activity that will cause you to get your heart rate elevated. Increased blood flow to the surgical site can cause bleeding problems, swelling and excessive scarring.
Swelling is common following Mohs Surgery, particularly when the surgery is performed around the eyes, cheeks and forehead. Usually this is not a problem. Bruising is common 3-4 days after the surgery. The instruction sheet includes information on how to take care of yourself and the area of surgery. We do insist on daily cleaning and dressing changes.
The surgery site will be wider and deeper than the area that was biopsied. It can be as small as a dime or often larger than a quarter and extend into the fatty tissue.
When Dr. Johnson/ Dr. Miller/ Dr. Strahan has determined that the skin cancer has been completely removed, a decision is made on what to do about the wound created by the surgery. Usually there are four choices:
Dr. Johnson/ Dr. Miller/ Dr. Strahan will recommend which of these choices will be best for your individual case. The final decision is yours.
Follow-up visits for at least five years are essential with either Dr. Johnson/ Dr. Miller/ Dr. Strahan or your referring physician. After the wound has healed, patients return at three months, six months and one year. There are two reasons that this is important.
First, if there is recurrence of the skin cancer it may de detected and treated at once. It has been shown that if there is a recurrence it usually occurs with the first year following surgery.
Second, studies have shown that once you develop one skin cancer you are at higher risk for developing more in the years to come.
Therefore if you notice any suspicious areas, it is important that you bring it to the attention of either your referring doctor, Dr. Johnson, Dr. Miller or Dr. Strahan.
No, not entirely. We do not think that sunshine will be harmful to you as long as you take precautions. As mentioned earlier, sunlight is probably the main factor in development of skin cancer, and patients who have had one skin cancer often develop more at a later date. Therefore, in the future when you go into the sun, we recommend that you apply a sunscreen of SPF 15 or more to all exposed areas, including the lobes of the ears. Be sure to reapply it liberally after swimming or exercising, since most sunscreens wash off with water or perspiration.
In addition to a sunscreen, you should wear a hat.
Yes, you can lead a normal lifestyle, if you take precautions. Remember, an ounce of prevention is worth a pound of cure.
If you are taking any of the medications listed below, for headaches, menstrual cramps, etc. We strongly recommend that you switch to Tylenol for any of the above symptoms for 7 days before your surgery. If you are taking aspirin or aspirin containing products at the advice of your doctor to prevent strokes or heart attacks, please check with him or her as to the advisability of stopping these medications for the 7 day period prior to surgery. We generally find the doctor will be agreeable with stopping these.
If you are taking Coumadin (or any other blood thinner), please inform us. Please consult with your physician before stopping any prescribed medications.
The medications we recommend you not take are:
Arthritis Pain Formula
4-way- Cold Tablets
5A.S.A.
Advil
Alcohol
Aleve
Alka Seltzer
Anacin
Anaprox
Anaproxin
APC
Ascodeen
Ascriptin
Aspergum
Aspirin
Brufen
Bufferin
Butazolidin
Celebrex
Cephalgesi
Cheracol Capsules
Children’s Aspirin
Clinoril
Congesprin
Cope
COQ10
Corididin
Coumadin (warfarin)
Darvon
Daypro
Dolobid
Dristan
Easpirin
Ecotrin
Empirin
Emprazil
Excerdin
Feldene Fiorinal
Fish oil
Gingko-Biloba
Goodies-Powder
Haltran
Ibuprofen
Indocin
Indomethacin
Meclomen
Medipren
Midol
Motrin
Nalfon
Naprosyn
Norgesic
Nuprin
Orudis
Phenaphen
Relafen
Rufin
Sine Aid
Trandate
Trental
Trigesic
Trilisa
Tumeric
Vanquist
Vitamin E
Voltarin
Zactri
Zorprin
Please also inform us well in advance of your surgery if you have a pacemaker, hip replacement or any other type of surgery that may necessitate prophylactic antibiotics to prevent Endocarditis (Heart valve complications) prior to surgery.
With recent changes in the insurance industry, we would like to clarify current insurance coverage for follow-up appointments after procedures. If you believe you have a potential complication after your Mohs procedure, such as an infection or any other possible problem, it is most important that you call our office so you can be optimally cared for. You health is our first priority!
If a flap closure is used (skin rotate in to repair the are) or a skin graft (skin taken from one site and moved to another site to repair it), the procedure and all associated care related to that procedure are bundled and included in the initial procedure fee for 90 days from the date of the procedure.
If a line of stitches is placed (intermediate or complex layered closure), the procedure and further care to that site are bundled and included in the initial procedure fee for 10 days. Suture removal with a Medical Assistant after 10 days would be a no-charge visit. Further care after that visit would be billed as an office visit, with any associated co-pays due at the time of service.
If you have chosen to let the surgical area fill in or “granulate in”, or a “Simple Repair” (such as a purse-string suture to partially close the area, or fenestration of cartilage, or altering the edges of the wound to change the angle), then any follow-up appointments would result in an office visit with associated co-pays due at the time of service. To be sure you are off to a good start, and all your questions for wound care have been addressed, we would not charge any fees for the first wound check.
Mohs Surgical Department